The fetus and children are more sensitive to ionising radiation exposure than adults.
It is well known that high doses of ionising radiation can cause harm, but there is continuing scientific uncertainty about effects at low doses. At levels of dose routinely encountered by members of the public and most present-day radiation workers, there is little or no epidemiological evidence of health effects. Radiation protection standards recognise that it is not possible to eliminate all radiation exposure, but they do provide for a system of control to avoid unnecessary exposure and to keep doses in the low dose range.
What are some obvious effects of ionising radiation exposure?
Extreme doses of radiation to the whole body (around 10 sievert and above), received in a short period, cause so much damage to internal organs and tissues of the body that vital systems cease to function and death may result within days or weeks. Very high doses (between about 1 sievert and 10 sievert), received in a short period, kill large numbers of cells, which can impair the function of vital organs and systems. Acute health effects, such as nausea, vomiting, skin and deep tissue burns, and impairment of the body’s ability to fight infection may result within hours, days or weeks. The extent of the damage increases with dose. These effects are called 'deterministic’ effects and will not be observed at doses below certain thresholds. By limiting doses to levels below the thresholds, deterministic effects can be prevented entirely.
How does ionising radiation affect human tissue?
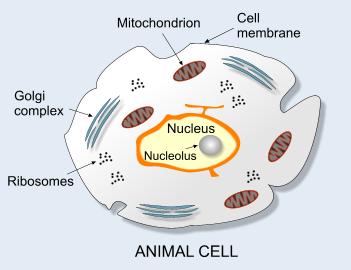 The body is made up of different cells. For example we have brain cells, muscle cells, blood cells etc. The genetic material of the cell is found in the nucleus in the form of genes which are in turn combined into strand-like structures called chromosomes. It is the genes within a cell that determine how a cell functions. If damage occurs to the genes then it is possible for a cancer to occur. This means the cell has lost the ability to control the rate at which it reproduces. If genes are damaged in reproductive organs a mutation may occur. Such a mutation may be passed on to children.
The body is made up of different cells. For example we have brain cells, muscle cells, blood cells etc. The genetic material of the cell is found in the nucleus in the form of genes which are in turn combined into strand-like structures called chromosomes. It is the genes within a cell that determine how a cell functions. If damage occurs to the genes then it is possible for a cancer to occur. This means the cell has lost the ability to control the rate at which it reproduces. If genes are damaged in reproductive organs a mutation may occur. Such a mutation may be passed on to children.Cancers and heritable mutations are called stochastic (probabilistic) effects. The cancer or mutation behaves the same whether the organ received a high absorbed dose or a low one, all that changes are the odds (probability) of a cancer forming or a mutation occurring. There are no types of cancers that are formed only as a result of radiation. Some types of cancers, however, show a bigger rate increase for a given radiation dose than others. Cancer risks are also known to vary with age at exposure and attained age, with risks being higher for those exposed as children.
Doses below the thresholds for deterministic effects may cause cellular damage, but this does not necessarily lead to harm to the individual: the effects are probabilistic or ‘stochastic’ in nature. There is good epidemiological evidence – especially from studies of the survivors of the atomic bombings - that, for several types of cancer, the risk increases roughly linearly with dose. There is statistically significant risk in the range 0 - 100 millisievert and useful risk estimates for doses as low as 50 - 100 millisieverts. The risk factor averaged over all ages and cancer types is about 1 in 10,000 per millisievert. The risk of inducing a heritable mutation is estimated to be about 2* in 100,000 per millisievert. Because of the chance nature of cell damage, not everyone who is exposed to the same amount of radiation will get cancer.
The fetus and children are more sensitive to radiation exposure than adults. An absorbed dose to the fetus of 100 – 500 millisievert can cause developmental problems such as malformation or reduced IQ.
While these studies indicate evidence of radiation-induced effects, epidemiological research has been unable to establish unequivocally that there are effects of statistical significance at doses below a few tens of millisieverts. Nevertheless, given that no threshold for stochastic effects has been demonstrated, and in order to be cautious in establishing health standards, the proportionality between risk and dose observed at higher doses is presumed to continue through all lower levels of dose to zero. This is called the linear, no-threshold (LNT) hypothesis and it is used for developing radiation protection standards.
What if an ionising radiation dose is received over a long period of time?
There is evidence that a dose accumulated over a long period carries less risk than the same dose received over a short period. Except for accidents and medical exposures, doses are not normally received over short periods, so that it is appropriate in determining standards for the control of exposure to use a risk factor that takes this into account. While not well quantified, a reduction of the high-dose risk factor by a factor of two has been adopted internationally, so that for radiation protection purposes the risk of radiation-induced fatal cancer is taken to be about 1 in 20,000 per millisievert of dose for the population as a whole.
* Hereditary Effects of Radiation, UNSCEAR 2001 Report to the General assembly, with Scientific Annex


